Fund Info
Time to get your physical exam
To enable members to receive a lower calendar- year deductible, in 2023, the Board of Trustees instituted an annual physical exam requirement for those on self-funded medical plans offered by the Automotive Industries Welfare Plan. The participant and their spouse or domestic partner (if applicable) who get an annual physical exam will be moved to the lower deductible level along with all dependent children. The physical exam can be taken any time before the end of the 2026 calendar year (December 31).
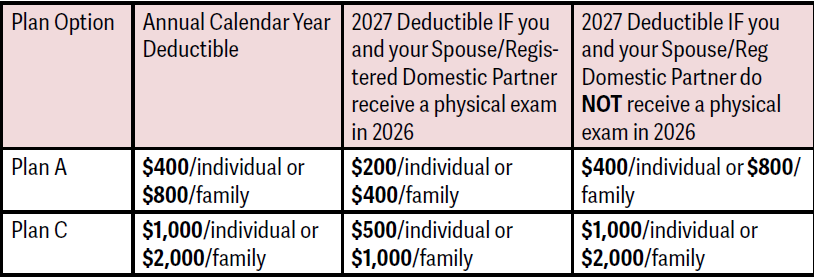
You’ll have to submit a Physical Exam Certification Form. A separate form must be submitted for you and your spouse or domestic partner (if applicable) to reduce your deductible for the 2027 calendar year. Forms have been mailed or may be obtained online at www.aitrustfunds.org. If you have questions about what deductible level you are in, please contact the Trust Fund Office at 800-635-3105 or by email at AISupport@ hsba.com.
Voluntary Wellness Program available
The Fund has a voluntary wellness program available to all participants and eligible spouses in the Automotive Industries Welfare Fund. The program is administered according to federal rules permitting employer-sponsored wellness programs that seek to improve employee health or prevent disease, including the Americans with Disabilities Act of 1990, the Genetic Information Nondiscrimination Act of 2008, and the Health Insurance Portability and Accountability Act, and others.
Employees who choose to participate in the wellness program will receive an incentive of a lower annual deductible. If you choose to participate in the wellness program, however, you will be asked to have a complete physical exam during Calendar Year 2026. Although you are not required to have the physical exam, only employees who do so will receive lower deductible in 2027.
The information from your physical exam will be used to provide you with information to help you understand your current health and potential risks.
Protections from Disclosure of Medical Information
We are required by law to maintain the privacy and security of your personally identifiable health information. Although the wellness program and Automotive Industries Welfare Fund may use aggregate information it collects to design a program based on identified health risks in the workplace, the Fund will never disclose any of your personal information either publicly, or to the employer, except as necessary to respond to a request from you for a reasonable accommodation needed to participate in the wellness program, or as expressly permitted by law. Medical information that personally identifies you that is provided in connection with the wellness program will not be provided to your supervisors or managers and may never be used to make decisions regarding your employment.
Your health information will not be sold, exchanged, transferred, or otherwise disclosed except to the extent permitted by law to carry out specific activities related to the wellness program, and you will not be asked or required to waive the confidentiality of your health information as a condition of participating in the wellness program or receiving an incentive. Anyone who receives your information for purposes of providing you services as part of the wellness program will abide by the same confidentiality requirements. The only individual(s) who will receive your personally identifiable health information is the Fund in order to provide you with your decreased deductible under the wellness program.
In addition, all medical information obtained through the wellness program will be maintained separate from your personnel records, information stored electronically will be encrypted, and no information you provide as part of the wellness program will be used in making any employment decision. Appropriate precautions will be taken to avoid any data breach, and in the event a data breach occurs involving information you provide in connection with the wellness program, we will notify you immediately.
You may not be discriminated against in employment because of the medical information you provide as part of participating in the wellness program, nor may you be subjected to retaliation if you choose not to participate.
If you have questions or concerns regarding this notice, or about protections against discrimination and retaliation, please contact the Fund Office at 800-635-3105 or by email at AISupport@ hsba.com.
Pension Plan Searching for Former Participants
About 2,000 participants are entitled to receive a pension payment under the Automotive Industries Pension Plan but have not made application for their money. If you know someone who used to work in the industry during the 1970s or 1980s, is over age 65, and is not receiving a pension payment from the Trust Fund, they could be missing out on a monthly payment from the Plan. Have them contact the Trust Fund Office at 800-635-3105 for a review of their work history to see if they are eligible.
Reminder: Update Your Address with the Trust Fund Office
You should update your address with the Trust Fund Office within 30 days of moving to your new residence.
You can submit your address change directly through the Trust Fund website at www.aitrustfunds.org by logging onto your personal account and completing the online form.
Health and Retirement Benefits
If you are looking for information about your health and pension benefits, please contact:
Automotive Industries Trusts Funds
Health Services & Benefit Administrators
4160 Dublin Boulevard, Suite 100
Dublin, CA 94568-7756
Phone (800) 835-3105
Email: AISupport@hsba.com
Website: www.aitrustfunds.org
IAM National Pension Fund
1300 Connecticut Avenue, NW, Suite 300
Washington, DC 20036-1711
Phone: 1-800-424-9608
Email: iamcontact@iamnpf.org
Website: www.iamnpf.org
IAM introduces new Group Medicare Plan
The IAM has worked for months to negotiate a new Group Medicare plan for Medicare-eligible retirees, spouses, surviving spouses and Medicare-eligible dependents.
In October, the IAM announced a new partnership with Employee Benefit Systems and TLC Insurance Group. This plan can help serve the Medicare needs for our Medicare-eligible retirees, their spouses, and surviving spouses. This new best-in-class IAM Group Medicare Advantage plan, offered through Humana, is rich in benefits.
Visit iam4.me/iamhumana for more information.
Here are some of the benefits that IAM retirees are so excited about:
• Available in all 50 states, plus Puerto Rico and the District of Columbia;
• National Passive Group Medicare PPO Plan that allows members to use the doctor and hospital of their choice nationally;
• In-network and out-of-network benefits are identical;
• Robust Prescription Group Plan included;
• Low out of pocket maximum;
• No deductibles on the IAMAW Group plan;
• Low copays! Primary Care Physician – $0 copay Specialist – $30 copay
By now, you should have received an announcement letter, followed by a group enrollment packet with details on the new group plan. If you have questions, feel free to call the Humana Enrollment Department toll free at 1-800-833-2411 for questions and enrollment assistance.
Retiree participation is not mandatory. Enrollment into the plan is by self-choice. The IAM recommends that all retirees compare the benefits of this new IAM Group Medicare plan with their current coverage prior to making any decision on their 2021 Medicare healthcare options. Visit iam4.me/iamhumana for more information.
Fund Info Archive
You’ll always have access to all Fund Info articles.